When a tooth is significantly compromised, the clinical path forward isn’t always clear. You weigh the remaining structure, occlusal forces, and the patient’s long-term prognosis. While a direct restoration might seem like the conservative choice, it can sometimes be a short-term fix for a long-term problem. The decision to place a dental crown is a commitment to providing 360-degree protection and restoring a tooth to full function for years to come. It’s about choosing predictability and strength when the biology and biomechanics demand it. This guide walks through the critical factors in that decision, from assessing structural integrity to selecting the right materials for a lasting, esthetic result.
Choosing between dental bonding vs. crown is a question of biology, biomechanics, and behavior. The strongest plan preserves sound structure, manages load, and delivers esthetics that hold up under daily function without constant chairside tweaks.
What is a Dental Crown?
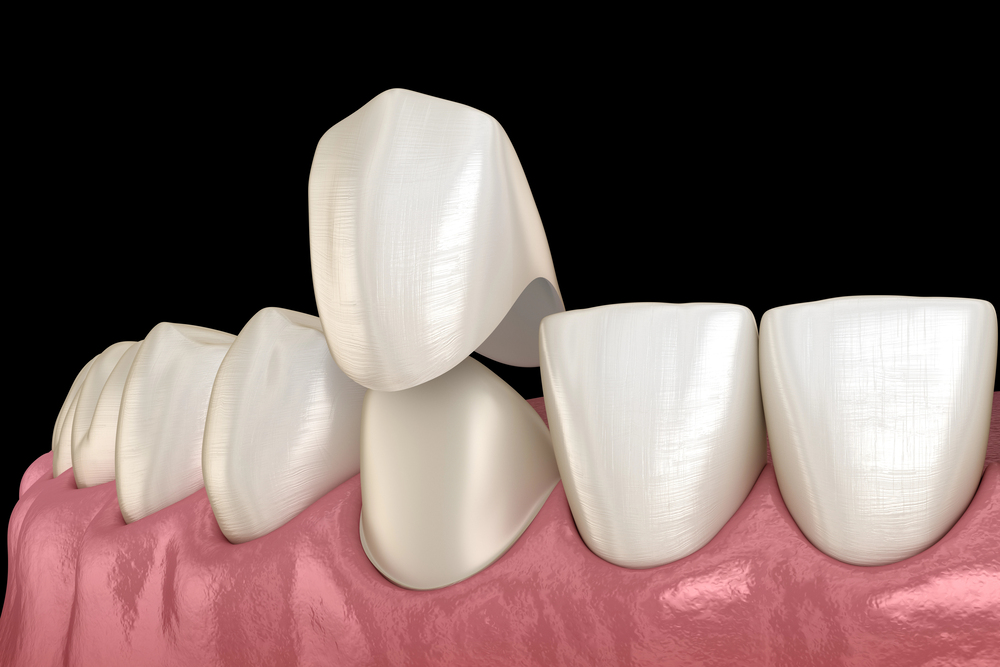
When a tooth is too damaged for a simple filling but doesn’t need to be extracted, a dental crown is often the best path forward. I like to think of it as a custom-made helmet for a tooth, providing 360-degree protection. As the Cleveland Clinic puts it, a crown is a “tooth-shaped cap” that restores a tooth’s shape, size, and strength while improving its appearance. This restoration encases the entire visible portion of the tooth down to the gum line, becoming its new, durable outer surface. It’s a foundational treatment in restorative dentistry, designed not just to patch a problem but to fully rehabilitate a tooth’s function and aesthetics for years to come.
Today’s crowns are crafted from advanced materials like porcelain, ceramic, and zirconia, each offering a unique balance of strength and aesthetics. The goal is always to create a restoration that looks completely natural while standing up to daily chewing forces, and material science has made this more achievable than ever. As a full-service lab, we see firsthand how critical the right material selection is for a successful, long-lasting outcome. Whether your priority is the supreme translucency of an anterior e.max crown or the brute strength of posterior zirconia, choosing the appropriate crown and bridge restoration ensures you can deliver a result that perfectly matches your patient’s clinical needs and cosmetic goals.
Common Indications for a Crown
Knowing when to opt for a crown over a more conservative treatment comes down to assessing the tooth’s long-term structural needs. A crown is the right call when a less-invasive restoration simply won’t provide enough strength or protection. As Healthdirect explains, they are ideal for teeth that are broken, cracked, severely decayed, or have undergone a root canal. They also solve major cosmetic issues that bonding can’t handle. Essentially, if a tooth is too weak to function reliably on its own, a crown provides the 360-degree reinforcement it needs to get back to work.
The decision to place a crown often arises from a few common clinical situations. When you need to provide comprehensive protection and restore full function, a crown is your most reliable tool. The Cleveland Clinic highlights several key indications for a crown, which include the need to:
- Make a weak tooth stronger.
- Protect a cracked tooth from further damage.
- Fix a tooth that’s broken or severely worn down.
- Hold a dental bridge securely in place.
- Cover a tooth that’s badly stained or discolored.
- Protect a tooth after a root canal treatment.
- Complete a dental implant restoration.
First, Assess the Tooth’s Structure and Stress
 Assessment begins at the tooth, not the material. Small chips, diastemas, and shallow cervical defects favor additive strategies. Large MODs, undermined cusps, and endo access signal a need for coverage. The occlusal scheme matters too. Deep overbites, heavy group function, and bruxism push toward protective designs that redistribute force and reduce flexure at thin walls.
Assessment begins at the tooth, not the material. Small chips, diastemas, and shallow cervical defects favor additive strategies. Large MODs, undermined cusps, and endo access signal a need for coverage. The occlusal scheme matters too. Deep overbites, heavy group function, and bruxism push toward protective designs that redistribute force and reduce flexure at thin walls.
When is Dental Bonding the Right Choice?
Composite bonding excels at conservative contouring, margin camouflage, and quick repairs. It is ideal for closing black triangles, lengthening worn edges slightly, masking localized discoloration, and reshaping peg laterals. In posterior teeth, selective bonding can repair corners or minor marginal breakdown without committing to full coverage. Advantages include single-visit delivery, minimal prep, favorable economics, and easy touchups or reversibility. With careful isolation, layered opacity control, and polished finishes, chairside esthetics can be outstanding.
What Are the Limits of Dental Bonding?
Bonded edges fatigue under high cyclic load. Long incisal additions on bruxers chip and stain. Wide posterior spans with missing marginal ridges flex, opening microgaps and inviting recurrent decay. Subgingival margins that bleed compromise bonding, and deep shades may require opaquer layers that add complexity. When the substrate lacks ferrule-like strength, bonding trades immediate beauty for medium-term maintenance.
Why a Dental Crown Might Be the Better Option
Crowns protect compromised teeth by covering cusps and stabilizing remaining walls. Post-endo molars, teeth with wide MODs, and cracks that cross marginal ridges benefit from coverage that lowers flexural stress. Partial coverage options, like onlays and overlays, can conserve structure while delivering the same protective effect. For patients with parafunction, full-contour zirconia or modern lithium disilicate can balance toughness, polishability, and esthetics.
Understanding the Benefits and Risks of Crowns
When the structural integrity of a tooth is significantly compromised, a crown offers a predictable and durable solution. However, like any restorative procedure, it comes with its own set of benefits and considerations that you’ll need to weigh with your patient. A crown is a significant investment in a tooth’s future, so walking through the pros and cons helps set clear expectations for the treatment’s success and longevity. It’s about finding the point where the need for protection outweighs the desire for maximum conservation of tooth structure.
Key Benefits of Dental Crowns
A dental crown is a custom-fit cap that covers the entire visible portion of a tooth, acting as its new external surface. This approach is incredibly effective for restoring teeth that are severely decayed, broken, or worn down. Crowns are also the standard of care for protecting teeth after root canal therapy or for completing a dental implant restoration. According to the Cleveland Clinic, this full-coverage design not only restores the tooth’s original shape and function but also protects the remaining structure from further damage. By distributing occlusal forces evenly, a well-made crown can significantly extend the life of a compromised tooth, making it a reliable and lasting solution in your restorative toolkit.
Potential Risks and Complications
The primary consideration for any crown is the necessary removal of natural tooth structure to create space for the restorative material. While this is essential for a strong and esthetic result, it’s an irreversible step. Patients may also experience some temporary sensitivity to hot or cold in the weeks following the procedure. Over the long term, potential issues can include the porcelain chipping, the crown becoming loose, or in rare cases, falling off entirely. As noted by Healthdirect, there’s also a risk of new decay forming at the margin of the crown if oral hygiene is not maintained, which underscores the importance of a precise fit from the lab and clear instructions for the patient.
Lifespan and Durability
While crowns are not a permanent fix, they are a long-term solution designed to last for many years. On average, a dental crown can last between five and 15 years, but with excellent patient home care and regular check-ups, it’s not uncommon for them to last much longer. The longevity of a crown is a team effort, depending on the patient’s habits, the precision of your clinical work, and the quality of the restoration itself. Modern materials, like the high-strength zirconia and lithium disilicate we work with, offer impressive durability that stands up to years of function, giving you and your patients confidence in the final result.
Matching the Right Material to the Case
- Anterior esthetics: lithium disilicate crowns offer translucency and strength for moderate load zones, while bonding handles minor contour and shade blending with minimal removal.
- Posterior durability: full-contour zirconia resists fracture and wears the antagonist gently when polished, while composite patches in high load areas invite frequent refinements.
- Mixed cases: a hybrid plan may place a crown on a crack-prone molar while using bonding for small anterior esthetic tweaks.
All-Ceramic or All-Porcelain Crowns
When aesthetics are the top priority, all-ceramic or all-porcelain crowns are often the best choice. They offer the most natural look, mimicking the translucency and color of real teeth, which makes them perfect for anterior restorations. This option is also ideal for patients with metal allergies, providing a biocompatible solution without compromising on appearance. Materials like Zirconia have become a go-to in this category, delivering exceptional strength that is also gentle on opposing dentition. By choosing a high-quality ceramic, you can provide your patients with a restoration that is both beautiful and durable, blending seamlessly into their smile.
Porcelain-Fused-to-Metal (PFM) Crowns
Porcelain-fused-to-metal crowns have long been a reliable standard in restorative dentistry, offering a combination of strength and aesthetics. They are built with a metal alloy interior for durability and are covered with a layer of porcelain that can be matched to the color of the patient’s natural teeth. While they are incredibly strong and long-lasting, they do have a few considerations. The porcelain layer can sometimes chip or fracture, and PFM crowns may cause more wear on the opposing teeth. Over time, the metal margin can also become visible as a dark line at the gumline, which can be an aesthetic concern for some patients, particularly in the anterior region.
Metal Crowns
For posterior teeth that handle the brunt of chewing forces, nothing beats the durability of a full metal crown. Made from alloys containing gold, nickel, or chromium, these crowns are exceptionally strong, resistant to chipping, and incredibly long-lasting. One of their biggest clinical advantages is that they require less tooth structure to be removed compared to other crown types. The obvious trade-off is their metallic color, which is why they are almost exclusively reserved for out-of-sight molars. For patients who prioritize longevity and strength over aesthetics in the back of the mouth, a metal crown is a fantastic and predictable option.
All-Resin Crowns
All-resin crowns are typically the most cost-effective option available, but that lower price point comes with significant trade-offs in terms of durability. Made from a dental composite resin material, these crowns are more prone to fractures and wear down more quickly than their porcelain or metal counterparts. Because of their lower strength, they are not usually recommended for long-term restorations on permanent teeth. Instead, their most common application is for temporary crowns that protect a prepared tooth while the final, more permanent restoration is being fabricated by the lab. Their expected lifespan is generally around three to five years.
How Gums and Margins Influence Your Decision
Healthy, accessible margins support both modalities. Supragingival finish lines favor predictable bonding and simplify hygiene. Subgingival defects complicate isolation and finishing for composites, raising the appeal of crowns with well-placed, cleansable margins. Tissue phenotype and biotype guide emergence design so papillae and cervical contours remain stable after healing.
Comparing Cost, Time, and Appointments
Bonding often wins on speed and upfront cost, making it suitable for interim smile upgrades, test drives for shape changes, or budget-limited plans. Crowns typically require more steps unless a same-day CAD-CAM pathway is available. Over a multiyear horizon, fewer repairs and better load distribution can make a crown more economical for severely compromised teeth. Share both timelines so patients understand maintenance expectations.
The Crown Placement Process
When you’ve determined a crown is the best clinical choice, the next step is walking the patient through the placement process. The workflow generally follows one of two paths: the traditional two-visit method or a single-visit appointment using in-office CAD/CAM technology. Both have their place in a modern practice, and the decision often comes down to your office’s equipment, the complexity of the case, and patient preference. Explaining the timeline and what to expect during each appointment helps manage patient expectations and builds trust in your treatment plan.
The Two-Visit Approach
The conventional method for placing a crown remains a reliable standard of care. The first appointment is dedicated to preparation. You’ll prepare the tooth, ensuring adequate clearance for the restorative material, and then take an impression. Whether you’re sending a traditional PVS impression or a digital scan, this is where your lab partner fabricates the custom restoration. You’ll fit the patient with a temporary crown to protect the tooth while the lab works. In the second visit, typically a couple of weeks later, you’ll remove the temporary, try in the permanent crown to verify fit and esthetics, and then permanently cement it.
Single-Visit CAD/CAM Options
For practices equipped with chairside milling units, you can offer patients the convenience of a single-visit crown. This process uses CAD/CAM technology to design, mill, and deliver the crown in one appointment, eliminating the need for a temporary restoration and a second visit. While this is an excellent option for many cases, it requires a significant investment in technology and training. For practices that prefer to outsource fabrication, partnering with a lab that thrives on digital workflows can significantly shorten turnaround times and still deliver precise, beautiful results without the overhead of in-office milling.
Factoring in the Cost of Treatment
Discussing cost is a critical part of treatment planning. For patients, a dental crown can cost anywhere from $500 to $3,000 per tooth, and dental insurance plans often cover a portion of this expense. The final fee you present to the patient reflects your chair time, clinical expertise, and overhead, which includes the lab bill. Working with a lab that provides high-quality crown and bridge restorations at a competitive price point can make a significant difference. It allows you to manage your practice’s costs effectively while making essential treatments more accessible for your patients, ensuring they can choose the best clinical option without cost being the only barrier.
Guiding Patients on Crown Aftercare
Once the final crown is cemented, the conversation naturally shifts to aftercare. Setting clear expectations helps patients feel confident and reduces post-op calls. Let them know it’s completely normal to experience some sensitivity to hot or cold for a couple of weeks as the tooth and surrounding tissues settle down. The gums might also be a little sore for a few days following the procedure, but over-the-counter pain relievers are usually enough to manage any discomfort. Reassure them that they can typically return to their normal activities right away, though they may want to chew on the opposite side for the first 24 hours.
Long-term care is just as important as immediate post-op instructions. Emphasize that a crown needs the same diligent care as a natural tooth. This includes brushing twice a day and, crucially, flossing daily to keep the margin where the crown meets the tooth clean and free of plaque. You can recommend they use a floss threader or interdental brush if access is tricky. A high-quality, well-fitted crown and bridge restoration is designed for longevity, but its success ultimately depends on the patient’s commitment to oral hygiene. Advising them to avoid chewing on extremely hard things like ice or hard candy can also prevent unnecessary fractures and ensure the restoration lasts for years to come.
Addressing Common Patient Concerns
Proactively addressing potential issues is key to building patient trust. It’s helpful to give patients a short list of things to look out for after their crown is placed. Encourage them to call your office if they notice the crown feels loose, as this could allow bacteria to seep underneath and cause decay. Similarly, a persistent bad taste or odor around the crown might indicate a problem with the seal or gum health. While modern ceramic materials are incredibly strong, they aren’t indestructible. Tell patients to check for any chips or cracks, especially after eating something hard.
Another common issue is irritation from the crown’s shape. If a patient reports that a sharp edge is bothering their tongue or cheek, it’s a simple fix that can be smoothed out in a quick office visit. By arming your patients with this information, you empower them to be active partners in their oral health. It shows you care about their long-term comfort and the success of the treatment. According to the American Dental Association, proper fit and maintenance are crucial, and clear communication ensures patients know exactly how to care for their new restoration and when to seek your help.
Explaining the Crown vs. Veneer Distinction
Patients often use the terms “crown” and “veneer” interchangeably, so having a simple explanation ready is always a good idea. The easiest way to frame it is by function and coverage. A crown is like a helmet for the tooth; it covers the entire visible surface down to the gumline. Its primary purpose is to restore a tooth’s strength, shape, and function, though it certainly provides an aesthetic benefit. In contrast, a veneer is more like a press-on nail. It’s a very thin shell of porcelain that covers only the front surface of the tooth and is used almost exclusively for cosmetic enhancements like changing color, shape, or closing small gaps.
Discussing Treatment Alternatives
When a tooth is too damaged for a simple filling but doesn’t quite need a full crown, it’s important to discuss the “in-between” options. Inlays and onlays are excellent conservative alternatives that fit into a tooth like a puzzle piece, restoring a cusp or portion of the chewing surface without removing as much healthy tooth structure. If the patient’s concerns are purely cosmetic, like minor chips or discoloration on an otherwise healthy tooth, veneers are the more appropriate choice. And for teeth that are unfortunately beyond saving, the conversation shifts to extraction and replacement with a dental implant, which provides a permanent and highly functional solution.
Managing Post-Procedure Sensitivity
It’s wise to prepare patients for the possibility of temporary sensitivity after crown preparation and placement. Explain that the process can sometimes irritate the nerve inside the tooth, leading to a short-term reaction to temperature changes. This is a normal part of the healing process and usually subsides within a few weeks. You can suggest they use a desensitizing toothpaste during this period and try to avoid consuming extremely hot or cold foods and drinks. Reassure them that this sensitivity is temporary, but also advise them to call if it doesn’t improve after a few weeks or if it suddenly worsens, as that could indicate a different issue.
Partnering for Efficient, Esthetic Results
Partner with Next Dental Lab for crown and bridge restorations that balance strength, esthetics, and chairside efficiency. Options span full-contour zirconia for durable posterior work, layered zirconia for lifelike translucency, and high-translucent zirconia that blends beautifully without roughening opposing teeth. IPS e.max crowns bring glass-ceramic brilliance for conservative cases, while PFM choices in non-precious, noble, and high-noble alloys deliver toughness with tailored biocompatibility. Full-cast crowns remain a rock-solid option for long-term service. Send a case with photos and RX, and receive consistent fits, clean contacts, and on-time delivery from our lab team focused on practical, patient-ready outcomes.
Frequently Asked Questions
What’s the single biggest factor that pushes a case from bonding to a full-coverage crown? The decision often comes down to the loss of structural integrity, specifically when one or both marginal ridges are gone. A tooth with a wide opening across the top, like a large MOD preparation, has lost its natural hoop strength and is much more susceptible to fracture. While bonding can fill the space, it can’t adequately brace the remaining cusps against chewing forces. A crown provides 360-degree coverage that holds the tooth together, effectively restoring that lost strength and preventing catastrophic failure.
How can I best explain the long-term value of a crown versus the lower upfront cost of bonding to my patients? I find it helps to frame the conversation around investment and predictability. Explain that bonding is an excellent solution for smaller, additive repairs, but for a significantly compromised tooth, it’s more of a patch than a permanent fix. While a crown has a higher initial cost, it’s designed to rehabilitate the tooth’s function for many years. You can mention that the cost of repeatedly repairing or replacing a large bonding that is likely to chip or stain can eventually meet or exceed the one-time cost of a durable crown.
My patient has a structurally sound anterior tooth but wants a major shade change. Is a crown overkill? Yes, in most cases, a crown would be too aggressive for that situation. When the primary goal is cosmetic and the tooth is otherwise healthy, your most conservative and appropriate options are treatments like whitening or veneers. A veneer requires minimal preparation of only the facial surface, preserving the tooth’s natural strength. A crown, on the other hand, requires removing healthy tooth structure from all sides, which is unnecessary for a purely aesthetic enhancement on a strong tooth.
What’s the most common point of failure for crowns, and how can I minimize that risk from the start? The most vulnerable area is the margin where the crown meets the tooth. An open or poorly sealed margin allows bacteria and plaque to get underneath, leading to recurrent decay that undermines the entire restoration. The best way to prevent this is to ensure a precise preparation with clear finish lines, take a high-quality impression or digital scan, and partner with a lab that consistently delivers restorations with an impeccable fit. This clinical precision is the foundation for long-term success.
For posterior teeth, when should I choose zirconia over a PFM or full-cast metal crown? Full-contour zirconia has become the go-to for most posterior cases because it offers an ideal blend of strength and esthetics. It’s strong enough to withstand heavy chewing forces without the risk of porcelain chipping that you have with PFMs. While full-cast metal is incredibly durable, most patients today prefer a tooth-colored option. Zirconia provides that natural look without compromising the longevity needed for a molar, making it the most versatile and predictable choice for the back of the mouth.
Key Takeaways
- Assess the Tooth, Not Just the Blemish: The best treatment choice starts with the tooth’s structural integrity. Bonding is ideal for conservative, additive repairs on healthy teeth, while a crown provides essential 360-degree protection for teeth compromised by cracks, decay, or root canals.
- Match the Material to the Functional Zone: Select materials based on the specific demands of the case. Use highly esthetic options like lithium disilicate for anterior restorations where appearance is paramount, and rely on durable materials like full-contour zirconia for posterior teeth that handle heavy occlusal forces.
- Set Clear Expectations for Long-Term Success: A restoration’s longevity depends on patient partnership. Clearly communicate aftercare instructions, costs, and what to expect post-procedure to empower patients and ensure they properly maintain their new crown for years to come.
Related Articles
- Dental Bonding Vs. Dental Crown: Which Option Fits Your Patients Best?
- Dental Crown Vs. Filling: How Dentists Decide The Best Treatment
- Temporary Crown Vs. Permanent Crown For Patients: Which Delivers Better Outcomes?
- 5 Types of All Porcelain Crowns Explained
- Crown Vs. Extraction: Which Treatment Is More Effective For Your Patient?

